Cardiac auscultation is a cardinal skill in the battlefield of medicine, enable healthcare professionals to assess the heart's condition by heed to its sounds. This technique is essential for name diverse cardiac conditions, and mastering it involves understanding the key cardiac auscultation spots. These spots are specific areas on the chest where the stethoscope is placed to listen to the heart's sounds most efficaciously. This usher will delve into the importance of cardiac auscultation, the key spots, and the techniques involve in do this crucial diagnostic routine.
Understanding Cardiac Auscultation
Cardiac auscultation is the process of listening to the heart s sounds using a stethoscope. It is a non invading method that provides worthful information about the heart s function and can help in diagnosing various cardiac conditions. The heart produces respective sounds, include the familiar lub dub rhythm, which corresponds to the closing of the heart valves. By heed to these sounds, healthcare professionals can detect abnormalities such as murmurs, clicks, and gallops, which may indicate underlie heart issues.
The Importance of Cardiac Auscultation Spots
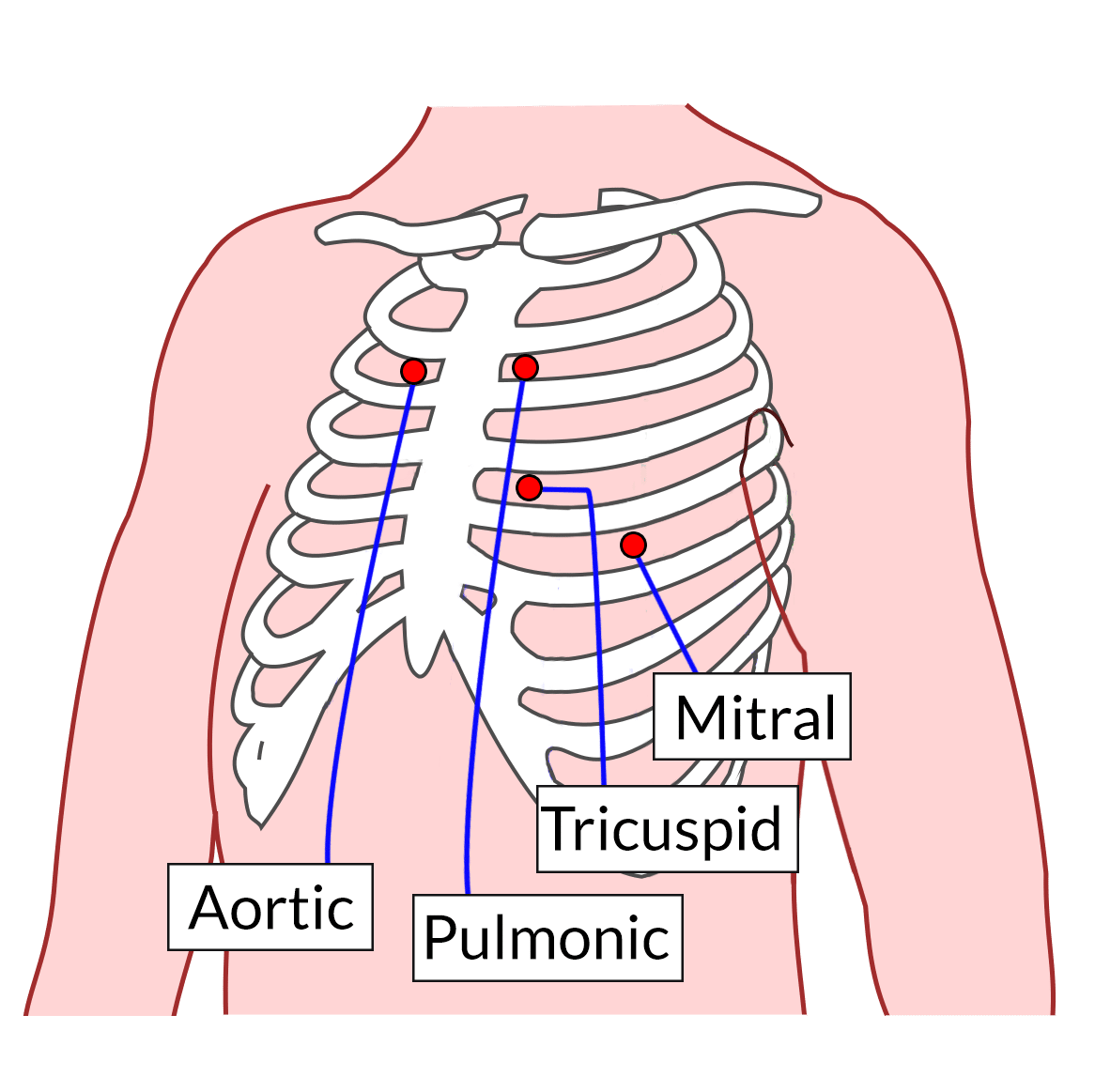
Identifying the correct cardiac auscultation spots is important for accurate diagnosis. The heart s sounds can be best heard at specific locations on the chest, known as auscultatory areas. These spots correspond to the valves and chambers of the heart, permit for precise assessment of each part. The main cardiac auscultation spots include:
- Aortic region: Located at the second right intercostal space, just to the right of the sternum.
- Pulmonic area: Located at the second left intercostal space, just to the left of the sternum.
- Tricuspid country: Located at the fourth left intercostal space, just to the left of the sternum.
- Mitral area: Located at the fifth left intercostal space, at the midclavicular line.
Techniques for Effective Cardiac Auscultation
To perform cardiac auscultation efficaciously, healthcare professionals must follow a taxonomic approach. This involves using the correct technique and listening for specific sounds at each cardiac auscultation spot. The following steps outline the process:
- Prepare the patient: Ensure the patient is comfortable and lying down in a quiet environment. Ask the patient to expose their chest and remove any tog that may obstruct the auscultation process.
- Position the stethoscope: Place the diaphragm of the stethoscope on the skin at the cardiac auscultation spots. Apply gentle press to control full contact with the skin.
- Listen to the heart sounds: Listen for the normal lub dub rhythm and any extra sounds such as murmurs, clicks, or gallops. Pay attention to the timing and quality of the sounds.
- Assess each auscultatory area: Move the stethoscope to each of the primary cardiac auscultation spots and listen for sounds at each location. Compare the sounds heard at each spot to identify any abnormalities.
- Document findings: Record the findings of the auscultation, remark any abnormal sounds and their characteristics. This information is essential for diagnosing and handle cardiac conditions.
Note: It is important to listen to the heart sounds in a quiet environment to avoid any outside noise that may interfere with the auscultation process. Additionally, ensure that the stethoscope is clean and in good work condition to find accurate results.
Common Cardiac Auscultation Findings
During cardiac auscultation, healthcare professionals may clash assorted sounds and rhythms. Understanding these findings is essential for accurate diagnosis. Some common findings include:
- Normal heart sounds: The familiar lub dub rhythm, which corresponds to the shut of the mitral and aortic valves (S1) and the shut of the pneumonic and tricuspid valves (S2).
- Murmurs: Abnormal sounds caused by turbulent blood flow through the heart valves. Murmurs can be systolic (occurring between S1 and S2) or diastolic (hap between S2 and the next S1).
- Clicks: Sharp, eminent pitch sounds that may indicate valve prolapse or other structural abnormalities.
- Gallops: Additional heart sounds that occur in rapid sequence, often bespeak heart failure or other cardiac conditions.
- Rubs: Scratching or grating sounds that may show pericarditis, inflammation of the pericardium.
Advanced Cardiac Auscultation Techniques
besides the canonical techniques, advanced cardiac auscultation methods can provide more detailed info about the heart s function. These techniques include:
- Dynamic auscultation: Listening to the heart sounds while the patient performs specific maneuvers, such as alter positions or make their breath. This can help place certain types of murmurs and other abnormalities.
- Phonocardiography: Recording the heart sounds using a specialized device telephone a phonocardiogram. This allows for detail analysis of the sounds and can aid in diagnosing complex cardiac conditions.
- Doppler echocardiography: Using ultrasound engineering to visualize the heart s structures and blood flow. This technique can supply valuable info about the heart s function and help in diagnose conditions such as valve stenosis or regurgitation.
Challenges in Cardiac Auscultation
While cardiac auscultation is a worthful symptomatic tool, it is not without its challenges. Some common difficulties include:
- Obese patients: Excess body fat can create it difficult to hear the heart sounds clearly. In such cases, using a larger stethoscope diaphragm or applying more pressure may help.
- Loud environments: Background noise can interfere with the auscultation process. Ensuring a quiet environment is essential for accurate results.
- Patient movement: Movement during auscultation can distort the heart sounds and make it difficult to prevail accurate readings. Asking the patient to remain still is crucial.
- Technical issues: A faulty stethoscope or improper technique can lead to inaccurate results. Ensuring the stethoscope is in good act condition and using the correct technique is crucial.
Training and Practice
Mastering cardiac auscultation requires practice and experience. Healthcare professionals should undergo thorough condition in cardiac auscultation techniques and practice regularly to meliorate their skills. Some tips for efficacious practice include:
- Use simulated patients: Practice on simulated patients or mannequins to familiarize yourself with the auscultation operation and different heart sounds.
- Listen to recordings: Use audio recordings of heart sounds to practice identifying normal and abnormal sounds.
- Seek feedback: Practice with experienced healthcare professionals and try their feedback to improve your technique.
- Regular practice: Incorporate cardiac auscultation practice into your routine to maintain and raise your skills.
Cardiac Auscultation in Different Patient Populations
Cardiac auscultation techniques may vary reckon on the patient population. for instance, auscultation in paediatric patients requires a smaller stethoscope diaphragm and a gentler approach. In elderly patients, auscultation may be more challenging due to conditions such as arthritis or obesity. Understanding the unparalleled needs of different patient populations is essential for effective cardiac auscultation.
Cardiac Auscultation in Special Situations
In certain situations, such as during pregnancy or in critically ill patients, cardiac auscultation may stage unique challenges. for case, in significant patients, the heart s position may shift due to the growing uterus, postulate adjustments in the auscultation technique. In critically ill patients, auscultation may be difficult due to the presence of aesculapian devices or the patient s status. Healthcare professionals must adapt their techniques to these situations to obtain accurate results.
Cardiac Auscultation and Technology
Advancements in technology have enhanced the capabilities of cardiac auscultation. Digital stethoscopes, for instance, can amplify heart sounds and filter out background noise, making it easier to detect abnormalities. Additionally, mobile apps and software can record and analyze heart sounds, providing worthful insights for diagnosis and treatment. Integrating engineering into cardiac auscultation can improve accuracy and efficiency, benefiting both healthcare professionals and patients.
Cardiac Auscultation in Clinical Practice
In clinical practice, cardiac auscultation is a routine part of the physical scrutiny. It is used to sort for cardiac conditions, reminder patients with known heart disease, and assess the effectiveness of treatments. Healthcare professionals should incorporate cardiac auscultation into their regular practice to guarantee comprehensive patient care. Regular auscultation can help in early detection of cardiac issues, stellar to well-timed intervention and punter outcomes.
Cardiac Auscultation and Patient Education
Educating patients about the importance of cardiac auscultation can heighten their realise of their heart health. Healthcare professionals should explain the auscultation process to patients, answering any questions they may have. This can help patients feel more comfy during the procedure and encourage them to seek regular check ups. Patient education is a important aspect of prophylactic care and can lead to wagerer health outcomes.
Cardiac Auscultation and Research
Research in cardiac auscultation continues to advance our understanding of heart sounds and their clinical implication. Studies have explored the use of hokey intelligence in analyzing heart sounds, the development of new auscultation techniques, and the wallop of auscultation on patient outcomes. Ongoing enquiry is all-important for improve diagnostic accuracy and developing innovative approaches to cardiac auscultation.
Cardiac Auscultation and Public Health
Cardiac auscultation plays a vital role in public health by enabling early spying and management of cardiac conditions. Regular auscultation in community settings, such as schools and workplaces, can assist name individuals at risk of heart disease. Public health initiatives that encourage cardiac auscultation can contribute to trim the burden of cardiovascular disease and better overall health.
Cardiac Auscultation and Global Health
In low resource settings, cardiac auscultation is a cost effective and approachable diagnostic tool. It can be used to screen for cardiac conditions in populations with limited access to advance medical technology. Training healthcare workers in cardiac auscultation techniques can amend the quality of care in these settings, stellar to bettor health outcomes for patients.
Cardiac Auscultation and Future Directions
The future of cardiac auscultation holds promise with the consolidation of engineering and innovative techniques. Advances in digital stethoscopes, unreal intelligence, and mobile health applications can enhance the accuracy and efficiency of auscultation. Continued research and development in this battlefield will pave the way for improved symptomatic capabilities and better patient care.
Cardiac Auscultation and Ethical Considerations
Ethical considerations in cardiac auscultation involve ascertain patient privacy, obtaining informed consent, and preserve professional standards. Healthcare professionals must respect patient autonomy and supply clear explanations of the auscultation operation. Adhering to ethical guidelines is crucial for building trust and see patient expiation.
Cardiac Auscultation and Interprofessional Collaboration
Effective cardiac auscultation requires coaction among healthcare professionals, including physicians, nurses, and technicians. Interprofessional teams can work together to perform auscultation, interpret findings, and develop treatment plans. Collaboration enhances the lineament of care and ensures comprehensive patient management.
Cardiac Auscultation and Patient Safety
Patient safety is paramount in cardiac auscultation. Healthcare professionals must postdate strict protocols to ensure accurate and safe auscultation. This includes using sterile equipment, sustain a clean environment, and cleave to infection control measures. Prioritizing patient safety is all-important for prevent complications and ensuring convinced outcomes.
Cardiac Auscultation and Quality Improvement
Continuous lineament improvement in cardiac auscultation involves regular training, feedback, and updates on best practices. Healthcare organizations should enforce quality improvement initiatives to enhance auscultation skills and ensure ordered execution. Quality improvement efforts can guide to better diagnostic accuracy and meliorate patient care.
Cardiac Auscultation and Patient Centered Care
Patient centered care in cardiac auscultation focuses on the individual needs and preferences of patients. Healthcare professionals should seamster auscultation techniques to each patient, considering factors such as age, sexuality, and medical history. Patient centre care promotes better communication, trust, and satisfaction, leading to improved health outcomes.
Cardiac Auscultation and Cultural Competency
Cultural competency in cardiac auscultation involves interpret and respect the cultural beliefs and practices of patients. Healthcare professionals should be aware of cultural differences that may affect auscultation, such as modesty concerns or language barriers. Cultural competency enhances patient provider communicating and ensures culturally sensitive care.
Cardiac Auscultation and Health Disparities
Addressing health disparities in cardiac auscultation involves providing equitable access to symptomatic services and reduce barriers to care. Healthcare professionals should be aware of the social determinants of health that may involve auscultation, such as socioeconomic status, pedagogy, and healthcare access. Efforts to reduce health disparities can improve the caliber of care and health outcomes for marginalized populations.
Cardiac Auscultation and Preventive Care
Preventive care in cardiac auscultation focuses on early detection and management of cardiac conditions. Regular auscultation can facilitate identify risk factors and prevent the advancement of heart disease. Healthcare professionals should accentuate the importance of prophylactic care and encourage patients to undergo regular check ups. Preventive care is essential for keep heart health and trim the risk of cardiovascular events.
Cardiac Auscultation and Chronic Disease Management
Chronic disease management in cardiac auscultation involves monitoring patients with known heart conditions and adjusting treatment plans as ask. Regular auscultation can help assess the effectiveness of treatments and detect any changes in the heart s function. Healthcare professionals should act closely with patients to manage inveterate conditions and ameliorate their quality of life.
Cardiac Auscultation and Emergency Care
In emergency care, cardiac auscultation is a critical instrument for rapid assessment and diagnosis. Healthcare professionals must be fix to perform auscultation in high stress situations and make quick decisions based on their findings. Effective auscultation in emergency settings can relieve lives and improve patient outcomes.
Cardiac Auscultation and Pediatric Care
Pediatric cardiac auscultation requires special considerations due to the unparalleled anatomy and physiology of children. Healthcare professionals should use smaller stethoscope diaphragms and gentle techniques to avoid make discomfort. Regular auscultation in paediatric patients can help detect inborn heart defects and other cardiac conditions early, leading to timely interference and better outcomes.
Cardiac Auscultation and Geriatric Care
Geriatric cardiac auscultation involves assessing the heart s function in older adults, who may have age pertain changes and comorbidities. Healthcare professionals should be aware of the challenges in auscultation, such as obesity, arthritis, and discover loss. Regular auscultation in geriatric patients can help grapple age related cardiac conditions and improve their quality of life.
Cardiac Auscultation and Women s Health
Cardiac auscultation in women s health involves see the unique cardiovascular risks and conditions that affect women. Healthcare professionals should be aware of gender specific factors, such as hormonal changes and pregnancy, that may affect auscultation. Regular auscultation in women can help detect conditions such as mitral valve prolapse and peripartum cardiomyopathy, leading to wagerer management and outcomes.
Cardiac Auscultation and Men s Health
Cardiac auscultation in men s health focuses on the cardiovascular risks and conditions that are more prevalent in men. Healthcare professionals should be aware of factors such as higher rates of hypertension and coronary artery disease in men. Regular auscultation in men can help detect conditions such as aortal stenosis and hypertrophic cardiomyopathy, leading to better management and outcomes.
Cardiac Auscultation and Mental Health
Cardiac auscultation and mental health are interconnect, as stress and anxiety can regard the heart s function. Healthcare professionals should consider the mental health status of patients during auscultation and provide reserve support. Addressing mental health concerns can improve overall health and well being, leading to punter cardiac outcomes.
Cardiac Auscultation and Lifestyle Factors
Lifestyle factors such as diet, exercise, and smoke can significantly impact cardiac auscultation findings. Healthcare professionals should assess these factors during auscultation and cater lifestyle modifications as want. Encouraging healthy lifestyle habits can amend heart health and reduce the risk of cardiovascular disease.
Cardiac Auscultation and Medication Management
Medication management is an essential aspect of cardiac auscultation, as certain medications can affect heart sounds and part. Healthcare professionals should review patients medication lists during auscultation and assess for any possible interactions or side effects. Proper medicament management can enhance the accuracy of auscultation and ameliorate patient outcomes.
Cardiac Auscultation and Follow Up Care
Follow up care in cardiac auscultation involves monitor patients after initial assessments and treatments. Regular postdate up auscultation can assist track the progress of cardiac conditions and adjust treatment plans as needed. Healthcare professionals should schedule postdate up appointments and provide ongoing support to ensure continuous care and improved outcomes.
Cardiac Auscultation and Patient Education
Patient didactics is a essential component of cardiac auscultation, as inform patients are more probable to adhere to treatment plans and maintain heart health. Healthcare professionals should ply open explanations of auscultation findings, answer patients questions, and proffer educational resources. Empowering patients with cognition can lead to better self management and better health outcomes.
Cardiac Auscultation and Communication
Effective communicating is all-important in cardiac auscultation, as it ensures accurate info exchange between healthcare professionals and patients. Healthcare professionals should use clear and concise language, fighting heed, and empathy during auscultation. Good communication can build trust, enhance patient satisfaction, and meliorate the quality of care.
Cardiac Auscultation and Documentation
Accurate documentation of cardiac auscultation findings is essential for patient care and continuity. Healthcare professionals should record detailed notes, including the auscultation technique, findings, and any abnormalities find. Proper support ensures that all healthcare team members are informed and can supply consistent care.
Cardiac Auscultation and Quality Assurance
Quality assurance in cardiac auscultation involves regular audits, feedback, and uninterrupted improvement. Healthcare organizations should implement quality assurance programs to monitor auscultation practices, place areas for improvement, and ensure bond to best practices. Quality assurance efforts can enhance the accuracy and dependability of auscultation, leading to punter patient outcomes.
Cardiac Auscultation and Evidence Based Practice
Evidence establish practice in cardiac auscultation involves
Related Terms:
- how to perform cardiac auscultation
- cardiac auscultation locations
- where to ascultate heart sounds
- auscultation of heart locations
- heart sounds where to listen
- where to assess heart sounds